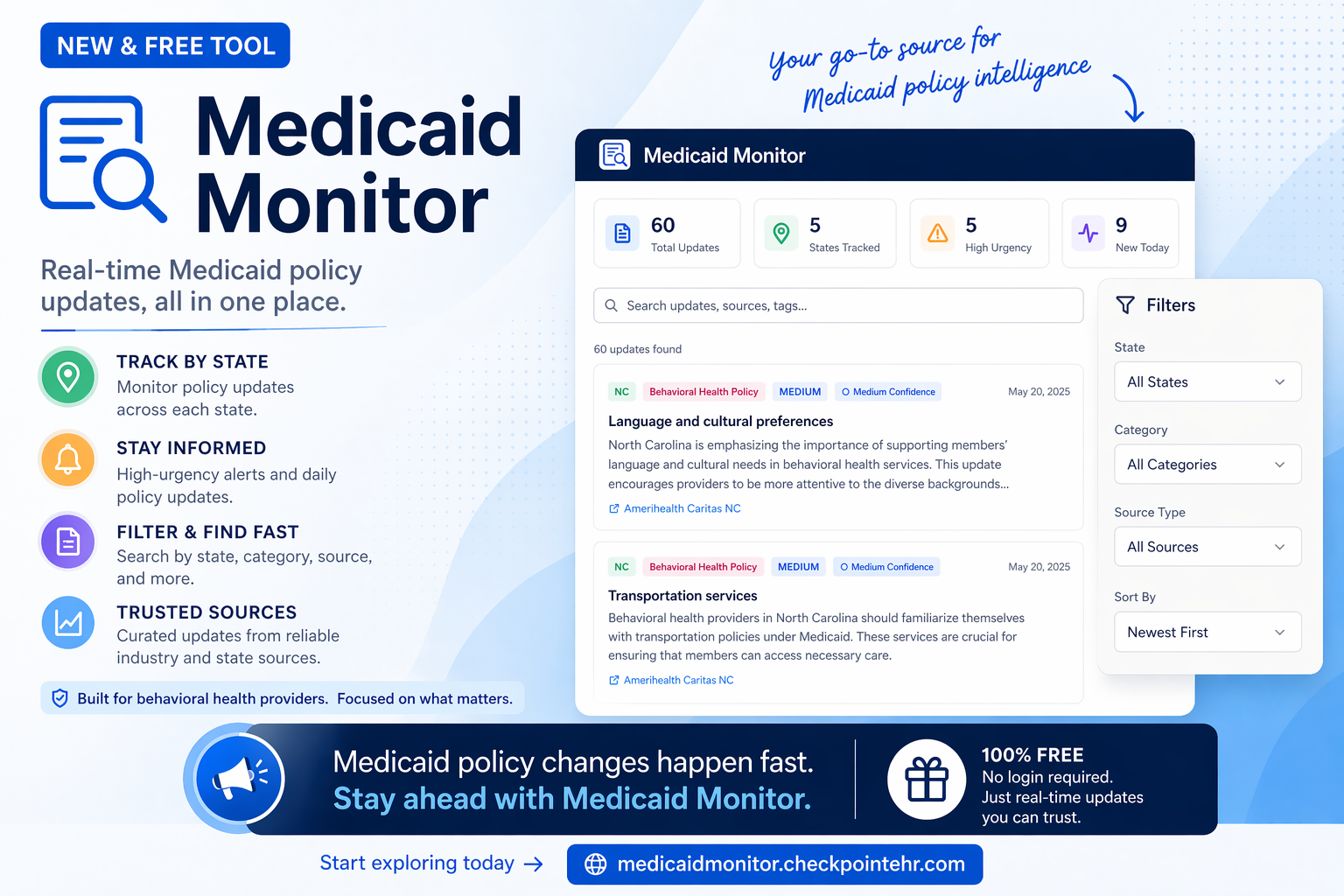
Your end-to-end electronic health record system.
Schedule a demo to see just how smooth your clinical operations can be at your practice.
No add-ons. Unlimited users. All features included.

Documentation
Easily manage all notes, intake, and paperwork.
Go paperless in all your client documentation.
Evaluate client information, symptoms, and patterns.
Create a comprehensive plan for client goals & interventions.
Easily enter multiple client's session notes at once.
Billing
Submit billing codes and claims with just a few simple clicks.
Customize billing code lists for your specific services.
Batch and automate daily claim submissions, hands-free!
Coming Soon!
Track all staff, client, claims, and financial data in one place.
Administration
Manage all clinician and client information in one place.
Quickly generate itemized staff payroll reports.
Track staff credentials to ensure licensures and trainings are renewed and up-to-date.
Easily track authorization units with payers to avoid denials.
Unlimited support from an assigned member of our success team.
Client Management
Provide your clients with the highest quality of care.
Centralize client communication, payments, and documentation.
Automate client notifications for appointments and important dates.
Chart client progress over time based on clinical interventions.
Easily transfer documentation for supervisor review.
Integrations
Take advantage of the software integrations centralizing your EHR experience.
Conduct virtual sessions via Zoom Healthcare integration.
Streamline documentation with AI progress notes assistant.
Seamlessly manage client prescriptions and medications.
Streamlining your claims review process with Availity.
Check out these Customer Stories
See how our practices, clinics, and agencies are benefiting from CheckpointEHR’s comprehensive features and therapist-friendly interface in this case study.
What people are saying...
“You are a wonderful team. We have tried EHRs before with different companies and they were not able to deliver, but Checkpoint is diligent, faithful, responsive, and always there. It is greatly appreciated. The entire office staff loves working with Checkpoint. It has really prepared us for expansion. The assistance you give is wonderful.”
Tamika
Business Manager

Join the Best Practice Therapist Newsletter!
Free behavioral health tips & resources delivered straight to your inbox. From clinical operations and organizational management, to scaling your practice and digital marketing, Best Practice Therapist provides you with practical tools & insights in 1-2 minute doses.
Looking to evaulate a new EHR system for your practice?
Get in touch with us today to learn more!