Join the Best Practice Therapist newsletter today → Subscribe
Outcome Measurements
Track Client Progress over time with an outcome measurement system that quantifies and timestamps client information and treatment responses.
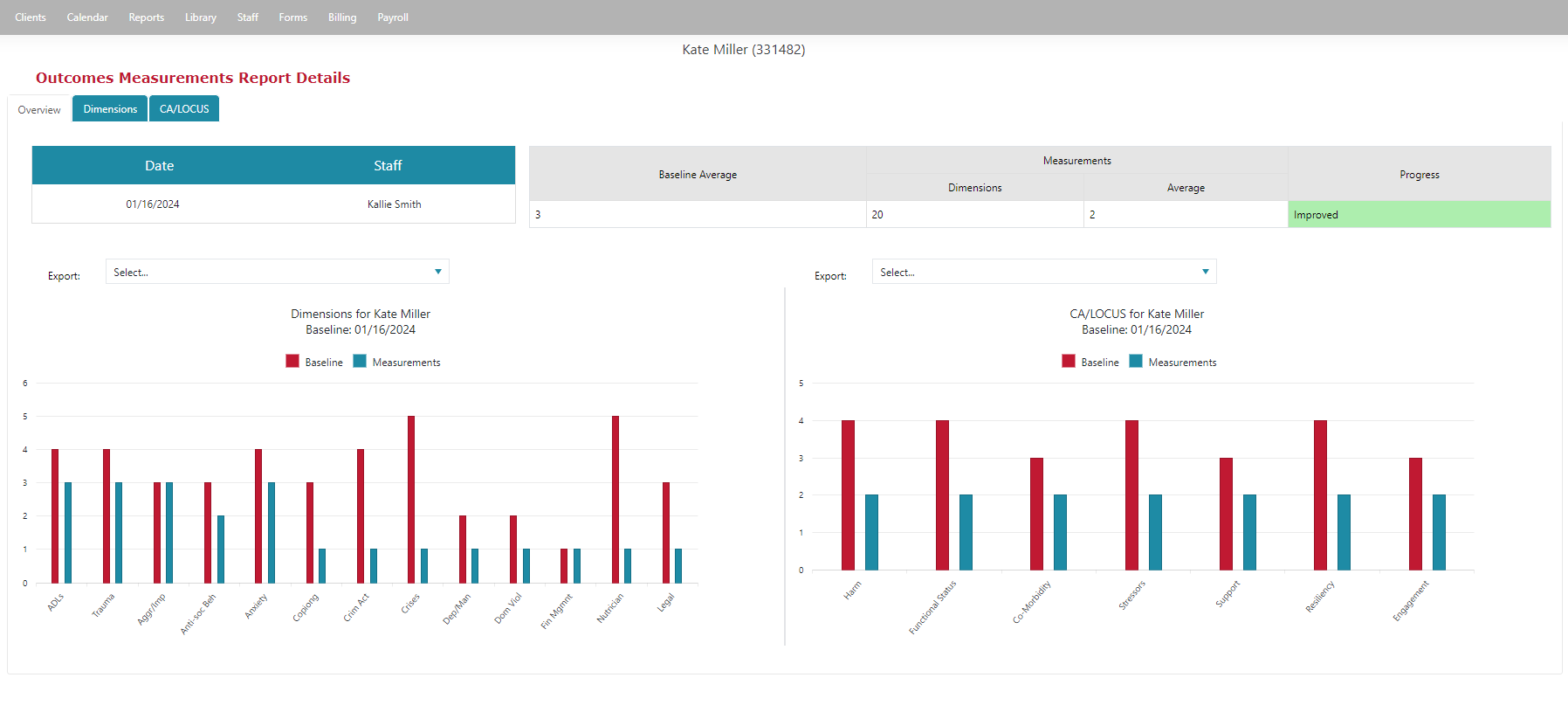
Track Progress with Outcome Measurements
Provide high-quality clinical services with measurement-driven care.
Rating Tools
User-friendly rating system to track quantifiable measures.
Dynamic Graphs
Visualize treatment & outcome progress with charts & graphs.
Track Progress
Time-stamped progress mapping of client outcomes.
Downloadable Files
Easily download & export outcomes in PDF & Excel.
Rating Tools
Seamlessly log updated client information and track assessment results over time using an outcome-based rating system to track client progress.
Dynamic Graphs
Visually depict all outcome measurement data using dynamic charts and graphs to capture client progress over time.


Track Progress
Monitor patterns and trends of each clients response to treatment over time with timestamped data that tracks their progress.
Downloadable Files
Need to download or export a clinical outcome measurement chart or graph? Now you can in both PDF and Excel formats.

Check out Janine's Story
See how Liaisons Wellness Center benefited from CheckpointEHR’s clinician-friendly EHR system in this case study.
What people are saying...
“You are a wonderful team. We have tried EHRs before with different companies and they were not able to deliver, but Checkpoint is diligent, faithful, responsive, and always there. It is greatly appreciated. The entire office staff loves working with Checkpoint. It has really prepared us for expansion. The assistance you give is wonderful.”
Tamika
Business Manager

Join the Best Practice Therapist Newsletter!
Free behavioral health tips & resources delivered straight to your inbox. From clinical operations and organizational management, to scaling your practice and digital marketing, Best Practice Therapist provides you with practical tools & insights in 1-2 minute doses.
Looking to evaulate a new EHR system for your practice?
Get in touch with us today to learn more!